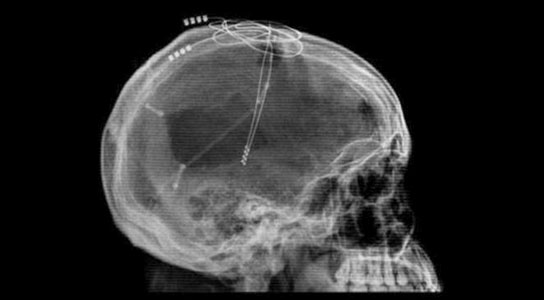
We’ve all heard of a pacemaker for the heart, but did you know there’s such a thing as a brain pacemaker? That’s not the official name of course; the brain pacemaker is more commonly known as deep brain stimulation or DBS for short. DBS is a system in which electrodes are implanted in the brain that receives small pulses of electricity to disturb abnormal brain patterns. It’s a treatment primarily in patients with illnesses affecting movement and memory, such as Parkinson’s Disease and Epilepsy. This system can significantly lessen symptoms of tremors, stiffness, and slowness.
DBS is considered an ‘alternative’ treatment for many memory-related disorders, but it’s been in use for over 20 years and is FDA approved. There have been more randomized controlled trials for DBS than any other procedure in neurosurgery. DBS is not a miracle cure or an easy procedure. It is still invasive brain surgery and does not cure an illness, it merely attempts to lessen the symptoms. Even so, lessening of symptoms for those with Parkinson’s or tremors can be an incredible quality of life upgrade. More than 160,000 people around the world have received the treatment, according to a 2019 study.
How does it work? There are three main components of the DBS system. First, there is a lead, which is a coated wire with electrodes attached to the tip. This is what is implanted in the brain. The lead connects the second part of the system, an extension, an insulated wire that connects the lead to the generator, the third part of the system. The small pulse generator (neurostimulator) is generally implanted near the collarbone and is what supplies the pulses of electrical current to the brain. A patient is given a handheld controller that can turn the DBS system on and off.
After the initial surgery, a patient waits a few weeks until their doctor programs the correct electrical signal. The settings often have to be re-adjusted many times until the optimal results are achieved. The battery in the neurostimulator lasts anywhere from three to five years, and then, the battery can be replaced in a simple outpatient procedure. Already progress is being made in creating longer-lasting batteries.
Aside from the incredible results DBS can produce in patients, brain pacemakers do not cause any permanent damage to the brain and the procedure can be reversed if needed. According to Nader Pouratian, MD, director of UCLA’s Neurosurgical Movement Disorders Program, many patients share the attitude that “they wish they had done it earlier.”
One of the most challenging aspects of utilizing DBS as a medical treatment is finding the correct placement in the brain for the electrodes. For movement and memory disorders, the electrodes are generally placed in areas of the brain that control these functions, called the thalamus and the basal ganglia. But finding the exact right place is difficult because each person’s neural networks are placed a bit differently. A new finding is now showing that using a personal functional brain map for each patient is probably better than using an aggregate of brain maps across people with the same disorder. However, this is expensive and time-consuming.
The future of the potential of DBS is exciting. What began as a medical breakthrough for illnesses affecting memory and movement, is now being used for psychiatric illnesses such as treatment-resistant depression and obsessive-compulsive disorder. DBS is also being studied for the treatment of chronic pain, phantom limb syndrome, addiction, and morbid obesity. There are also many advances being made to the system itself. One of the three primary DBS device manufacturers, Medtronic, recently released a breakthrough product called the Percept PC Neurostimulator, which is the first device that can monitor and track brain signals, as opposed to the previous neurostimulators which simply send electric pulses.
The market for ‘brain pacemakers’ is expected to reach 4.33 billion dollars by the year 2027, showing there is a lot of hope for what DBS can do for a myriad of people in the future.