When the ambulance bay doors at Adventist Health Simi Valley opened on a Tuesday evening, a team of caregivers was already waiting.
Moments earlier, first responders called ahead, let our team know that they were rushing to our hospital with a woman who was exhibiting symptoms of a stroke. Immediately, communicators initiated an overhead page at the hospital. Within minutes, a neurologist stood by. Imaging techs cleared the CT scanner to make it available for stat diagnostics. Pharmacists began mixing crucial clot-busting medications. Meanwhile, nurses, doctors, lab technicians, and others were already assembled at the ambulance bay doors to meet the patient and immediately go to work assessing whether this was a stroke or a false alarm.
That type of immediate, coordinated response is critical with stroke, which occurs when a clot blocks the blood supply to the brain. Hospitals across the nation, including ours, however, have been taking fewer of these types of calls since the COVID-19 pandemic was first announced. Meanwhile, there is no indication that fewer people are suffering from strokes, leaving us gravely concerned about the health of our community.
Strokes are the fifth leading cause of death in the United States, killing about 140,000 people each year, according to the U.S. Centers for Disease Control and Prevention. What many do not realize is that it is also a leading cause of long-term disability, reducing mobility in more than half of stroke survivors older than 65.
That is why it is imperative for those experiencing symptoms to immediately call 9-1-1 and be transported to the nearest hospital for treatment. Stroke victims should never drive themselves to a medical facility. First responders are trained to recognize stroke symptoms and trigger the notification system that gets hospital staff ready, and that extra time is crucial. Every minute of a stroke kills about 2 million brain cells. It is why we say: “time is brain.”
At Adventist Health Simi Valley, we are an advanced primary stroke center, meaning we are able to treat patients with clot-busting drugs like Alteplase or TPA, have neurologists on standby 24 hours a day, and that our nurses hold national certifications on how to care for stroke patients.
It should go without saying that we do not want our friends and neighbors suffering from strokes. Some factors are out of our control, like age, genetics and family history, but others can be controlled.
Limit alcohol intake; reduce your blood pressure if it is high; keep your cholesterol down; stop smoking cigarettes, or other illicit drugs; and talk with your physician about a moderate exercise regimen. If you have diabetes, work with your doctor to get it under control. Roughly 80 percent of strokes are preventable, according to the American Heart Association.
All these risk factors can be easily modified with a little effort and working to control them could save your life.
STROKE SIGNS:
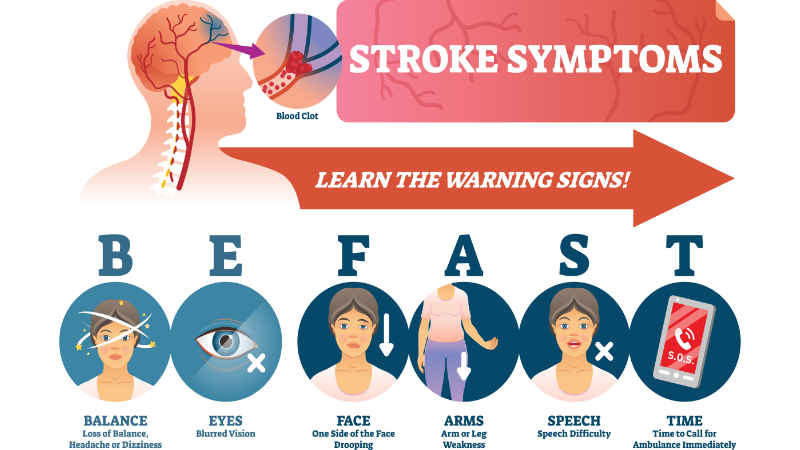
Recognizing stroke symptoms is critical when it comes to getting treatment quickly. Symptoms often come on suddenly, and can be remembered by the acronym, “BE FAST.”
B – Balance: Many stroke victims are thrown off balance.
E – Eyes: Blurred vision is common for stroke victims.
F – Face: The face often begins to droop to one side.
A – Arms: Arms sometimes fall to one side.
S – Speech: Stroke victims slur speech or are unable to speak.
T – Time: Time to call 9-1-1 if the above symptoms are observed.
Shannon Morris is a registered nurse and the stroke coordinator at Adventist Health Simi Valley.